Keloids Removal in New York
Get Rid of Stubborn Scar Tissue
Keloids are exaggerated scars that expand outside of the area of trauma, injury, or surgical scar. Scars are a natural part of the healing process. Keloid scars are an exaggeration of that normal healing response. These scars may form in response to trauma (burns, piercings or acne), injury, or surgical scars. Keloids look like large red/purple, solid nodules. They may also be itchy or tender. The likelihood of developing keloids is genetically determined- in predisposed people, keloids occur even with the most careful wound care. Keloids occur more commonly in African Americans.
Keep in mind that keloids are stubborn scars that tend to come back after treatment. The earlier a keloid scar is treated, the higher the chance it will respond to therapy! The therapy of choice is commonly an injection of a corticosteroid into the scar. The corticosteroid prevents the abnormal proliferation of the cells that form the scar. These steroid injections can make the flattened keloid appear better and less noticeable but will feel different than the surrounding skin.
Pulsed dye laser therapy is another option. The laser causes the keloid scar to get smaller by stopping the cells from multiplying. Combining laser treatment with corticosteroid injection is more effective than just laser therapy alone. Surgical excision (removal) is another choice and is also best followed by the injection of a corticosteroid.
Be sure to tell Dr. Rokhsar about the injury that caused the keloid and when you noticed it. In order to determine the best therapy, also tell the doctor if you have ever had any keloids treated in the past, either successfully or unsuccessfully.
Earlobe Keloids
Earlobe keloids appear as smooth, globular growths on one or both sides of the earlobe and may or may not be painful. They range in color from pink to red and may develop from an injury or wound site and can migrate into surrounding areas. Type of treatment depends on the location, size, depth, and duration of the earlobe keloid. The reason some people are more susceptible to keloid formation is currently unknown, but do occur more commonly in people with darker skin, those with body piercings, and the elderly more than children.
Keloids develop most often on the chest, back shoulders and earlobes. Removing a keloid depends on the symptoms that accompany its appearance. A chronically itchy or irritating keloid can pose problems and depending on the location, can be cosmetically sensitive or embarrassing and even lead to disfigurement.
A cortisone injection is a type of steroid, almost identical to the cortisone produced within the body. It is a steroid used to reduce inflammation and when treating keloids, flattens them but doesn’t completely rid the body of the keloid.
Using VBeam to Treat Earlobe Keloids
Dr. Rokhsar could use VBeam laser because of its effectiveness at flattening keloids and making them look less red. This treatment is relatively painless because it uses specific wavelengths to target the vessels or pigment responsible for the keloid appearance. The procedure lasts for up to 30 minutes and could require one to five treatments in order to obtain desired results.
Surgery is an option for removing a keloid by first injecting it with steroids to decrease its appearance and then once removed pressure is applied and the wound is dressed. This is risky because cutting a keloid can trigger the formation of a similar or even larger keloid post-surgery.
Cryotherapy, which is the freezing of affected cells in order to destroy them, can be used, however, freezing keloids with liquid nitrogen may only flatten them and darken the site after treatment.
Interferon, a topical treatment; fluorouracil, a chemotherapy treatment; or radiation are also treatment options used to reduce or eliminate keloids. Treatment depends on your case of severity, location, depth, and duration and if they develop, you should consult with your doctor.
Keloids Removal Before and After
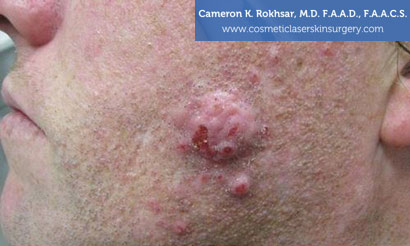
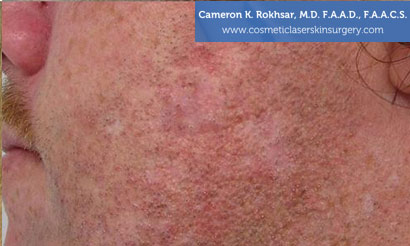
* Results May Vary
Keloids Removal FAQ
What causes keloids?
Keloids are raised overgrowths of scar tissue that occur at the site of skin injury or trauma. While the exact cause of keloids is not fully understood, several factors can increase the risk of developing them.
One of the main risk factors for keloids is having dark skin, particularly brown or Black skin. Other risk factors include a family history of keloids, pregnancy, age under 30 years old, and certain pre-existing skin conditions such as acne or chickenpox.
Keloids can occur from a variety of skin injuries, including cuts or punctures, burns, insect bites, surgical incisions, acne, tattoos, and body piercing. Keloids can also occur spontaneously, without any known injury, although this is rare.
It is thought that keloids occur due to an overproduction of collagen, which is the protein responsible for building scar tissue. This overproduction of collagen can lead to the formation of a keloid, which can continue to grow even after the wound has healed.
Treatment options for keloids include freezing with liquid nitrogen (cryotherapy), steroid injections, Kenalog/5FU injections, laser treatment, surgical removal, and radiation therapy. Keloids can be difficult to treat and may recur even after successful treatment.
How are keloids formed?
Keloids are formed from an overgrowth of scar tissue that occurs at the site of an injury or skin trauma, such as surgery, blisters, acne, tattoos, piercings, or minor scratches and bumps. The overgrowth is caused by an excessive production of collagen, which is a protein found throughout the body that is useful in wound healing. The exact reason why keloids develop is unknown, but they are more likely to occur in areas of the body that have more melanocytes (cells that make pigment), suggesting that melanin might play a role in causing keloids. Genetics is the largest contributing factor.
Keloids can be identified as smooth, hard growths that can be much larger than the original wound, and can range in color from pink to red/purple. They are more prevalent on the earlobes, jawline, chest, upper back, and shoulders, and may develop elsewhere on the body where the skin has been injured.
For newer keloids, the first treatment option might be compression dressings made from stretchy fabric or other materials, as this can reduce or prevent a scar by putting pressure on the wound as it heals. Other treatments include corticosteroid injections, 5FU injections, cryotherapy, laser therapy, radiation therapy, and surgical removal. However, keloids may recur after treatment, and not all treatments are suitable for every individual.
What does scar tissue look like?
Scar tissue can have various appearances depending on several factors such as the location of the scar, the type of injury, and the person’s age and skin type. Generally, scar tissue tends to be tighter and thicker than the surrounding skin. It may appear raised, sunken, lumpy, or flat and may be red, skin-colored, or darker than the surrounding skin. Scar tissue may also be painful, itchy, or cause limited movement if it forms a contracture scar.
Keloid scars are a type of raised scar that can form on tissues after an injury. They often appear on the upper body, particularly the chest, shoulders, and earlobes. Keloids are larger than the original wound, have a thick or lumpy appearance, and rise high above the rest of the skin.
Over time, scar tissue may change in appearance. Initially, the scarring may look minimal, but over 4-6 weeks, the scar may get bigger or become raised, firm, and thick. However, over the next 2-3 months, the scar may become smaller and blend in more with the surrounding skin.
In some cases, scar tissue can cause inflammation, redness, itchiness, throbbing, sensitivity to the touch, and reduced range of motion. Scar tissue fibrosis, a mass of hardened protein strands laid down haphazardly by fibroblasts at the injury site, is often a factor in chronic musculoskeletal pain.
How to soften scar tissue?
Scar tissue can often cause discomfort and restrict movement due to its stiffness and inflexibility. Fortunately, there are several ways to soften scar tissue and reduce its negative effects. Here are some methods that may be helpful:
- Massage: Physical therapists often use massage techniques like cross-friction and myofascial massage to soften scar tissue and reduce pain at the injured site. Massage also helps to improve blood flow and circulation to the area, promoting healing.
- Lubrication: Applying a small amount of oil, such as baby oil, vitamin E oil, or lotion, to the scar tissue can help keep it pliable and make it easier to massage. This can also prevent the scar from drying out and re-opening.
- Stretching: Stretching exercises, particularly those that involve the joint crossing the scar, can help to increase range of motion and reduce stiffness. Stretching can also promote blood flow to the area and improve overall flexibility.
- Medical treatments: For more severe scarring, medical treatments like laser therapy and steroid injections can be effective in reducing the appearance of scar tissue. A series of steroid/5FU injections is the most effective way to flatten raised keloids and decrease pain and itchiness in keloids. Dr. Rokhsar has successfully treated thousands of patients with stubborn keloids with a combination of steroid injections and laser procedures. If you are considering keloid removal, we recommend scheduling an appointment with Dr. Rokhsar to discuss your treatment options.
Scar tissue cannot be completely removed, but these methods can help to reduce its negative effects and improve mobility. Another fact is that keloids can recur even after treatment. Surgery has the highest recurrence rates out of any method.
How to prevent keloids?
Keloids are a type of raised scar that forms due to an overgrowth of collagen. They can be caused by various factors, including injury to the skin, burns, acne, or surgery. If you are prone to developing keloids, there are steps you can take to prevent them from forming:
- Protect the area from the sun: Exposure to the sun’s UV rays can worsen keloids, so it’s important to protect the affected area from the sun. Cover the area with clothing if possible, or use a sunscreen if clothing won’t cover the area when you’re outdoors. Dermatologists recommend using a tinted sunscreen if you have brown or black skin.
- Practice good wound care: Proper wound care can help prevent keloids from forming. Keep the wound clean and moist by gently washing the area with mild soap and water. Be sure to avoid injuring the skin, such as piercings, which can increase the risk of keloids.
- Use compression dressings: For newer keloids, the first treatment option might be compression dressings made from stretchy fabric or other materials. The goal is to reduce or prevent a scar by putting pressure on the wound as it heals.
- Apply silicone gel or sheets: Rub silicone gel or sheets onto the keloid for 2 to 3 minutes twice a day. Wait until the wound closes and then apply silicone gel onto the keloid. Use clean fingertips to massage the gel onto the keloid for 2 to 3 minutes. Then let the gel air dry. This can help flatten the keloid.
- Try corticosteroid injections: Dr. Rokhsar might recommend corticosteroid injections to reduce the size of the keloid. However, a possible side effect of these injections is light spots developing where you get these injections. If you have a darker skin tone, Dr. Rokhsar might use other medications including 5FU to prevent this.
- Consider other treatments: There are various other treatments that Dr. Rokhsar might recommend for keloids, including laser therapy and surgical removal. However, most keloids will return after surgical removal.
How to remove keloids?
While keloids are not harmful, they can be unsightly and cause discomfort, itching, and pain. Here are some ways to remove keloids:
- Injections: Corticosteroid injections, or Kenalog-5FU injections are the most effective treatment plan for keloids. They can shrink the scar when injected into the keloid. And decrease pain and itchiness. Repeat treatments may be needed.
- Cryotherapy: Freezing the scar tissue with liquid nitrogen may help reduce the appearance of keloids, although repeat treatments may be necessary. Possible side effects include blistering, pain, and hypopigmentation.
- Laser therapy: Pulsed-dye laser sessions, the Fraxel laser or fractional CO2 lasers can flatten larger keloids and fade their color. Laser therapy can also help flatten keloids on small areas.
- Surgery: Surgical excision, which removes the scar tissue, can flatten keloids. However, because it creates significant trauma to the skin, surgery may increase the likelihood of the keloid returning. Surgery should be avoided if possible due to high recurrence rates with keloids growing larger.
Removing keloids can be challenging, and not all treatments are effective for everyone. Prevention is the best approach for those prone to keloids. Taking precautions like protecting the skin from injury, especially after an ear piercing, can reduce the risk of getting a keloid.
How to get rid of piercing keloids?
Although keloids are not harmful, they can be uncomfortable, itchy, and unsightly. There are various treatment options available to help reduce keloids from piercings. Here are some of the options you can consider:
- Pressure earrings: Zimmer splints, also known as pressure earrings, can put pressure on the earlobe to reduce blood flow, which prevents the keloid from developing or coming back after treatment. Although they can be uncomfortable, wearing them for up to 16 hours a day for six to 12 months can be effective.
- Retinoids: Topical retinoids, such as tretinoin cream, can help reduce the size and appearance of keloids. However, they should only be used under the guidance of a dermatologist.
- Silicone gels: Several clinical studies found that using silicone gels on keloids has been found to be effective in reducing their appearance.
- Compression dressings: Compression dressings made from stretchy fabric or other materials can help reduce or prevent scarring by putting pressure on the wound as it heals. This method is also used after surgical removal of keloids.
- Laser treatment: Laser treatments with the Vbeam laser, Fraxel laser, or fractional CO2 lasers can help blend in the keloid scar and make it fade. The Vbeam laser is particularly effective for newer keloids.
- Cryotherapy: This treatment involves freezing the keloid, which can help reduce its hardness and size. However, it works best on small keloids.
- Corticosteroids: Corticosteroids are the gold standard for treating keloids. The medication can help shrink the keloid in size, but it usually takes approximately four to six injections every four weeks for the keloid to shrink significantly. Dr. Rokhsar combines his steroid injections with a drug called 5FU which aids in breaking down the keloid.
- Surgery should be reserved as a last resort for treatment of keloids.
How to get rid of keloids on the nose?
Keloids on the nose can be an unsightly and uncomfortable problem for some people. There are several treatments available that can help reduce the size and appearance of these scars. Here are some options to consider:
- Cryotherapy: This involves freezing the keloid with liquid nitrogen, which can reduce its size by up to 50 percent after several treatments. However, cryotherapy may cause side effects such as blistering, pain, and hypopigmentation.
- Laser treatment: Pulsed-dye laser sessions, Fraxel laser or fractional CO2 lasers can help flatten larger keloids on the nose. Laser therapy can also help fade the color of the scar well as blending the keloid in.
- Silicone sheets or gel: Wearing silicone sheets or gel over the scar can help flatten it.
- Corticosteroid injections: Dr. Rokhsar is often successful in flattening keloids with corticosteroid injections along with a special drug called 5FU.
No treatment can consistently get rid of a keloid, and what works for one person may not work for another. If you have concerns about a keloid on your nose, it is best to consult with Dr. Rokhsar for guidance on the best treatment options for your specific situation.
How to get rid of ear keloids?
Ear keloids often present as hard and in some cases painful nodules on ears. They often occur because of ear piercing or trauma and usually dangle from the ear lobe. It is most commonly seen in African Americans. Serial steroid injections are very effective in treating ear keloids. Combined with 5FU, the steroid injections become even more potent, often eliminating the need for surgery. Injections should be administered every four weeks. Surgical excision is another method to remove earlobe keloids. This is a 30 minute in-office surgery. Sutures are removed 10-14 days after surgery. Dr. Rokhsar recommends wearing pressure earrings right after suture removal to decrease the chance of the keloids growing back.
New York Office Locations
Upper East Side Manhattan Office
121 East 60th Street, Suite 8AB New York, NY 10022
(212) 285-1110
Long Island Office
901 Stewart Ave, Suite 240, Garden City, NY 11530
(516) 512-7616


 Dr. Rokhsar was chosen by
Dr. Rokhsar was chosen by 






