Skin Cancer Treatment in New York
- 1. What Are The 3 Different Types of Skin Cancer?
- 2. Squamous Cell Carcinoma
- 3. Melanoma Skin Cancer
- 4. How to Perform Self Skin Exams?
- 5. From head to toe
- 6. How Do You Identify Skin Cancer Lesions?
- 7. What Is The Most Common Treatment For Skin Cancer?
- 8. Mohs Surgery: Before and After
- 9. How Is Mohs Surgery Performed?
- 10. A Great Success Rate
- 11. About Mohs Surgery
- 12. Recovering From Mohs Surgery
- 13. Mohs Surgery FAQ
- 14. What Is The Mohs Surgery Healing Process Like?
- 15. Request an Appointment
- 16. New York Office Locations
What Are The 3 Different Types of Skin Cancer?
Basal Cell Carcinoma
There are several types of skin cancer, the most common being Basal Cell Carcinoma. This type most often occurs on the sun-exposed areas of the skin and may look like an open sore, reddish patch, or waxy growth with an elevated border and central indentation. Treatment of Basal Cell cancer includes excisional surgery, electrosurgery, microscopically controlled surgery, and radiation.
Squamous Cell Carcinoma
The second most common type of skin cancer is Squamous Cell Carcinoma. It also occurs most often on sun-exposed skin and may look like a scaly red patch with irregular borders, a wart-like growth, or an open sore. These cancers may bleed easily if bumped or disturbed. Treatments for this type of cancer include excisional surgery, electrosurgery, radiation, and microscopically controlled surgery.
Melanoma Skin Cancer
The most dangerous type of skin cancer is Melanoma. This may occur on any area of the body and may resemble a mole, but there are important differences. If you notice changes in a mole you should contact a physician immediately. A melanoma may present as an asymmetrical lesion with an irregular border. If the color or pigmentation of the area is not uniform, or if the diameter of the area is greater than six millimeters, these are also danger signs.
How to Perform Self Skin Exams?
An important aspect of detecting skin cancer early is performing self-exams of your skin. Make sure you have good light, either a full-length mirror (or a small chair or stool) and a hand mirror.
From head to toe
First, examine the face: pay special attention to the eyes (even behind the ears), lips, nose, and ears. Using a hand mirror will help you see both sides of the face.
With a hand mirror, check the scalp. The amount of hair you have will determine how long this step will take. Begin by making small parts in the hair and inspecting the scalp between the parts. Continue until you have inspected the entire scalp
Now, inspect the hands. Make sure to spread your fingers to check the interlacing skin. Check underneath the nails and the surface of the nails for any changes.
In front of the full-length mirror, survey the entire front of the body. It’s easiest to go top to bottom; so begin at the neck. If you are a woman, make sure to lift the breasts to inspect the skin underneath. Lift your arms over your head to see the skin under the arms and the skin on the sides of the body.
Turn around to examine the back of the torso. Use your hand mirror and start from the back of your neck and examine down the entire back.
Now, inspect the buttocks and the entire posterior surfaces of both legs.
Finally, examine the front of the legs and feet. For this step, you may feel more comfortable sitting down. Using your hand mirror, inspect the groin area, the front of the legs, the knees, and your lower legs. Moving down to the feet, examine the tops of the feet, the skin between the toenails, underneath the toenails, and the toenails themselves.
How Do You Identify Skin Cancer Lesions?
In addition to these three types of skin cancer, there are two types of lesions that have the potential to progress into skin cancer. One type of pre-cancer is Actinic Keratosis, which appears as a scaly or crusty bump and can be treated with curettage and Electrodesiccation, shave removal, dermabrasion, chemical peels, laser surgery, or topical medication.
The second type is the Dysplastic Nevi. Which are abnormal moles that resemble Melanoma and are often asymmetrical in shape, have an irregular border, vary in color, and are larger than normal moles. They should be watched carefully for changes that may indicate progressions to Melanoma.
It is important to remember that avoiding sun exposure and tanning beds and wearing sunscreen with an SPF of 30 or higher can best prevent these types of skin cancer.
What Is The Most Common Treatment For Skin Cancer?
Mohs Micrographic Surgery
There are five standard methods for the treatment of skin cancers. The two nonsurgical treatments are cryotherapy (deep freezing) and radiation therapy. Other methods include simple excision, physical destruction (curettage with electrodesiccation), and Mohs micrographic surgery. Newer techniques under investigation include photodynamic therapy and immunochemotherapy.
Treatment of each skin cancer must be individualized, taking into consideration such factors as patient’s age, the location of cancer, type of cancer, and whether or not cancer has been treated previously. In some instances, more than one type of therapy may be appropriate. But in most cases, only one or two are necessary for the particular type of skin cancer.
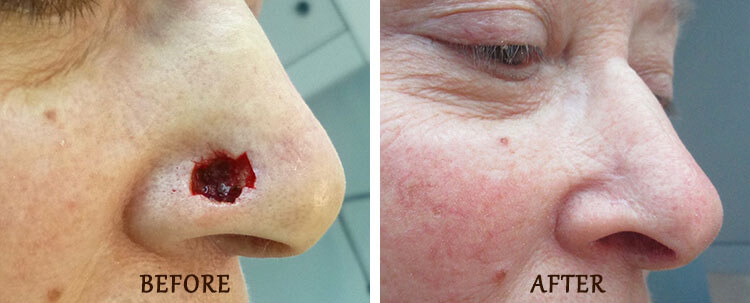
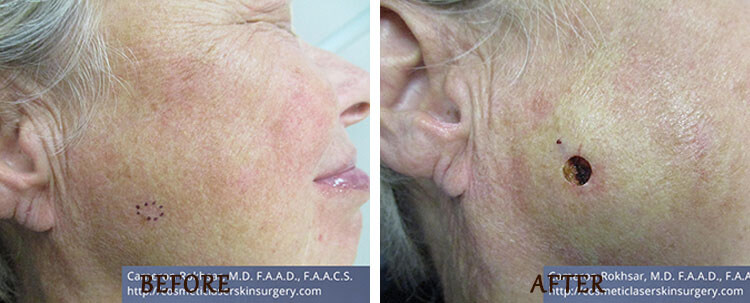
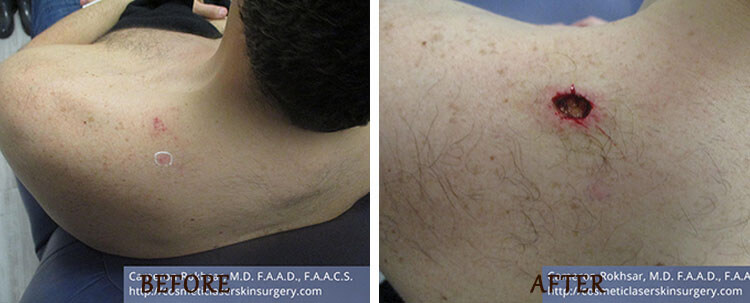
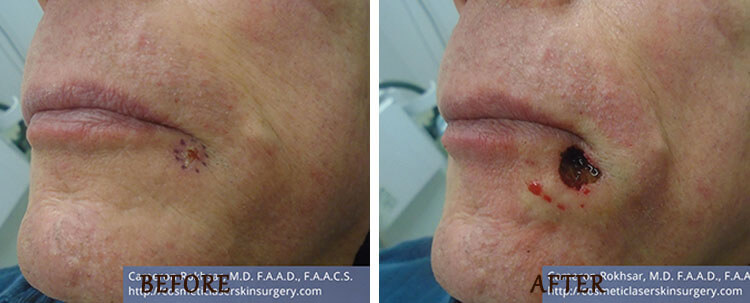
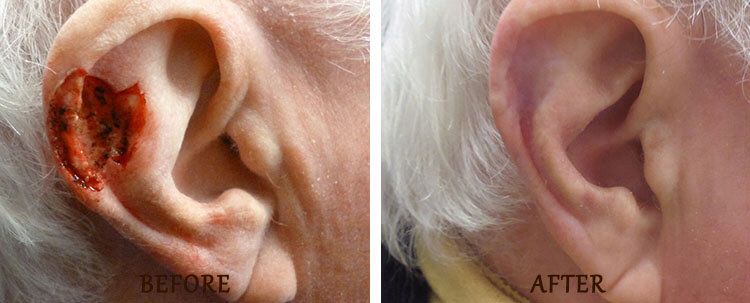
Mohs Surgery: Before and After
*Results may vary.
How Is Mohs Surgery Performed?
After the removal of the visible portion of the tumor by excision or curettage (debulking), there are two basic steps to each Mohs Micrographic Surgery stage. First, a thin layer of tissue is surgically excised from the base of the site. This layer is generally only 1-2 mm larger than the clinical tumor. Next, this tissue is processed in a unique manner and examined underneath the microscope.
On the microscopic slides, the entire bottom surface and outside edges of the tissue are examined. This issue has been marked to orient top to bottom and left to right. If any tumor is seen during the microscopic examination, its location is established, and a thin layer of additional tissue is excised from the involved area. The process is repeated until no tumor is found.
A Great Success Rate
Mohs Surgery in NYC allows for the selective removal of skin cancer with the preservation of as much of the surrounding normal tissue as is possible. Because of this complete systematic microscopic search for the “roots” of skin cancer. Mohs Micrographic Surgery offers the highest chance for complete removal of cancer while sparing the normal tissue. The cure rate for new skin cancers exceeds 97%.
As a result, Mohs surgery is very useful and may be recommended for the following types of cancer:
- When the size or extent of the skin cancer cannot be defined easily.
- When the cancer is in a place, such as a nose, eyelids, lips, or ears, where it is desirable to spare as much of the normal skin as possible.
- When cancer returns after being treated.
- When the cancer is large.
About Mohs Surgery in NYC
Mohs surgery has been shown to be a highly effective treatment for certain types of skin cancer, with a cure rate of up to 99% for certain tumors. Due to the fact that the Mohs procedure is micrographically controlled, it provides the most precise method for removal of the cancerous tissue, while sparing the greatest amount of healthy tissue.
For this reason, Mohs surgery may result in a significantly smaller surgical defect and less noticeable scarring, as compared to other methods of skin cancer treatment in NYC. The Mohs procedure is recommended for skin cancer removal in anatomic areas where maximum preservation of healthy tissue is desirable for cosmetic and functional purposes. It may also be indicated for lesions that have recurred following prior treatment, or for lesions that have the greatest likelihood of recurrence.
Recovering From Mohs Surgery
Your surgical wound will likely require care during the weeks following surgery. Instructions will be provided upon your Mohs Surgery at Dr. Rokhsar’s NYC office. You should plan on wearing a bandage and avoiding strenuous physical activity for a week. Most of our patients report minimal pain which is helped with Tylenol.
Patients may experience a sensation of tightness across the area of surgery since skin cancers frequently involve nerves and months may pass before your skin sensation returns to normal. In rare instances, the numbness may be permanent. Complete healing of the surgical scar takes place over 12-18 months. Especially during the first few months, the site may feel “thick,” swollen, or lumpy, and there may be some redness. Gentle massage of the area (starting about 1 month after the surgery) will speed the healing process.
Mohs Surgery FAQ
Will Mohs surgery leave a scar?
Mohs is a common surgical procedure to remove the layers of cancerous skin. It’s also the most precise technique for the removal of skin cancer. Dr. Cameron Rokhsar specializes in the treatment of skin cancer using the Mohs micrographic surgical technique. All surgical procedures have the potential for some degree of scar visibility. Dr. Rokhsar is also a leading expert in laser surgery treatments and can assure scarring will be minimalized. The appearance of a post-Mohs’ surgical scar depends entirely on the size, location, and skin type.
If skin cancer is in a noticeable facial area, should the Mohs Surgery be performed by a plastic surgeon?
Mohs surgery is a very delicate treatment that requires precision. It is advised skin cancer removal be performed by a dermatologist with specialized training in Mohs surgery. Dr. Cameron Rokhsar is a fellowship-trained dermatologist with specialized training in Mohs surgery and has performed countless procedures.
How should I prepare for Mohs Surgery?
Be well-rested and eat a good breakfast. Take your usual medications, unless directed otherwise. We request that you do not take any aspirin or aspirin-containing products, such as Anacin or Bufferin, for ten days prior to the surgery. In addition, please do not take Ibuprofen (Motrin, Advil, etc.). These medications may “thin” your blood and cause more bleeding. You may substitute acetaminophen (Tylenol) if required. Do not drink any alcoholic beverages for 24 hours before surgery.
What is skin cancer?
Skin cancer is a disease that occurs when the skin cells grow abnormally and out of control. There are three main types of skin cancer: basal cell carcinoma, squamous cell carcinoma, and melanoma. Basal cell carcinoma is the most common type of skin cancer, accounting for about 80% of all cases. Squamous cell carcinoma is less common but still represents a significant number of cases. Melanoma, while less common than the other two, is the deadliest form of skin cancer.
Skin cancers can appear in different ways, such as a new or changing mole, a red or scaly patch of skin, or a sore that does not heal. Skin cancers can develop anywhere on the skin but are most commonly found on areas that are frequently exposed to the sun, such as the face, neck, arms, and hands.
Not all skin cancers are caused by sun exposure. In some cases, skin cancer may develop due to genetic factors or exposure to certain chemicals. Regular skin checks by a board certified dermatologist are essential for early detection and treatment of skin cancer.
If you suspect you may have skin cancer or have noticed any changes in your skin, It is recommended to seek medical attention immediately. As a double board-certified dermatologist and skin cancer surgeon, Dr Rokhsar can provide comprehensive skin cancer screenings and treatment options, including Mohs surgery and surgical excisions for all forms of skin cancer. Remember, early detection and treatment can save lives.
What causes skin cancer?
Skin cancer is primarily caused by overexposure to ultraviolet (UV) radiation from the sun or other sources like tanning beds. When your skin is exposed to UV rays, it damages the DNA in your skin cells, leading to the formation of abnormal cells that can grow out of control and turn into cancer.
UV radiation can come from both UVA and UVB rays. UVA rays penetrate deep into the skin and can cause skin aging, while UVB rays affect the top layer of the skin and are the primary cause of sunburn. Both types of UV radiation can cause skin cancer.
Other risk factors that can contribute to the development of skin cancer include a family history of skin cancer, having fair skin, a history of severe sunburns or blistering, and exposure to certain chemicals or radiation.
It’s important to protect your skin from UV radiation by wearing protective clothing, seeking shade during peak sunlight hours, and using sunscreen with an SPF of 30 or higher. You should also have regular skin cancer screenings with a board certified dermatologist, especially if you have a family history of skin cancer or other risk factors. Early detection and treatment of skin cancer can lead to better outcomes and reduce the risk of complications.
What does skin cancer look like?
Skin cancer can take on many different appearances. It is important to be vigilant and aware of any changes in your skin, especially if you spend a lot of time in the sun or have a family history of skin cancer.
Some common types of skin cancer include basal cell carcinoma, squamous cell carcinoma, and melanoma. Basal cell carcinoma often looks like a flesh-colored, pearly bump or a pinkish patch of skin. Squamous cell carcinoma may appear as a persistent, red, scaly patch with irregular borders or a wart-like growth. Melanoma can vary in appearance but often looks like a changing mole with irregular borders, more than one color, and growing in size.
Other possible signs of skin cancer include persistent open sores, shiny bumps that can be pink, red, white or brown, patches of skin that are rough or scaly, and any mole or spot that changes in size, shape, or color.
It is important to have any suspicious skin changes evaluated by a board-certified dermatologist, who can perform a thorough examination and recommend the appropriate treatment. Early detection and treatment of skin cancer can greatly improve the chances of successful outcomes. Remember to protect your skin from the sun by wearing protective clothing and using sunscreen with at least SPF 30, and avoid tanning beds.
How fast does skin cancer grow?
There is no set timeline for skin cancer growth and appearance. Skin cancer can present in a variety of ways, including as a dark or large mole with uneven edges, a pimple or sore that does not heal within 2-3 weeks, a scaly spot, or a tender to sore spot. Skin cancers can present in a variety of colors, they can be dark or light, pink or brown.
Melanoma skin cancer, in particular, has a rapid growth rate, which is what makes it so dangerous. It can turn life-threatening in just six weeks and poses a high risk of spreading to other parts of the body if left untreated. The five-year survival rate for people with melanoma is about 99% if the cancer is detected early. But it drops to about 15% if cancer has spread to other parts of the body.
Basal and squamous skin cancer cells can also spread or metastasize to other parts of the body but this process usually takes a long time. By contrast, nodular melanomas can quickly grow and are more likely to invade other tissues than basal or squamous skin cancer.
Different types of skin cancer grow at different rates and that the growth rate can also vary depending on the location of the cancer. Basal cell carcinomas typically grow slowly, but they can be invasive and destructive over time. The location also matters. 2mm of growth on the nose or eyelid would have a greater impact.
Early detection is key when it comes to skin cancer. Dr. Rokhsar recommends that everyone performs regular self-examinations and visits a dermatologist annually for a full-body skin examination. If you notice any suspicious spots or changes in your skin, it is important to seek medical attention right away. Remember, prevention and early detection are key to keeping your skin healthy and cancer-free.
What are symptoms of skin cancer?
Skin cancer is a serious condition that affects people of all skin tones, including those with darker complexions. The most common sign of skin cancer is a change in your skin. This can be a new growth, a sore that doesn’t heal, or a change in a mole. Not all skin cancers look the same, and the specific signs and symptoms can vary depending on the type of skin cancer.
For melanoma specifically, a simple way to remember the warning signs is to remember the A-B-C-D-Es of melanoma. This stands for:
- A – Asymmetry: An irregularly shaped mole or growth.
- B – Border: A mole or growth with an irregular, scalloped, or poorly defined border.
- C – Color: A mole or growth with varying colors or shades of tan, brown, black, or even white, red or blue.
- D – Diameter: A mole or growth larger than the size of a pencil eraser (about 6 millimeters), although some melanomas can be smaller than this.
- E – Evolution: A mole or growth that looks different from other moles or growths on your skin, or that changes in size, shape, or color over time.
For basal cell carcinoma, signs and symptoms can include a sore or area of skin that doesn’t heal within 4 weeks, looks unusual, hurts, is itchy, bleeds, crusts or scabs for more than 4 weeks. This type of skin cancer can also appear as a slow-growing bump, sore-like growth, or rough-feeling patch on the skin.
Other types of skin cancer, such as squamous cell carcinoma, may initially appear as a nodule, rash, or irregular patch on the surface of the skin that may ooze or bleed easily. As the cancer grows, the size or shape of the visible skin mass may change and the cancer may grow into deeper layers of the skin.
It is important to perform regular self-exams of your skin to check for any new or changing moles or growths. If you notice any suspicious changes, it is important to see a dermatologist for evaluation and possible biopsy. Early detection and treatment are key to successful management of skin cancer.
What are the types of skin cancer?
There are three main types of skin cancer: basal cell carcinoma, squamous cell carcinoma, and melanoma. Basal cell carcinoma is the most common type of skin cancer, and it typically appears as a flesh-colored or pinkish bump on the skin. Squamous cell carcinoma is the second most common type of skin cancer, and it often appears as a scaly or crusty patch of skin. Melanoma is the least common but most dangerous type of skin cancer, and it can appear as a dark, irregularly shaped mole or spot on the skin.
Other, less common types of skin cancer do exist, but they are not as frequently encountered as these three main types. If you notice any unusual or suspicious changes in your skin, such as the appearance of a new growth, a change in the size or color of an existing mole or spot, or any other skin irregularities, it’s important to have them evaluated by a board-certified dermatologist. Early detection and treatment are key to successfully treating skin cancer, so don’t delay seeking medical attention if you have any concerns. Remember, prevention is also key, so always protect your skin from harmful UV radiation by wearing protective clothing and using sunscreen.
How dangerous is skin cancer?
Skin cancer is a serious condition that should not be taken lightly. The type of skin cancer and its stage determines how dangerous it can be. Actinic keratoses, for instance, are precancerous lesions that increase the risk of developing squamous cell carcinoma skin cancers. Melanoma is the most dangerous form of skin cancer because it can spread to other parts of the body if left untreated or caught in its late stages.
However, the good news is that if caught early, skin cancer can be cured with high success rates. Regular skin exams, self-examinations, and prompt attention to any changes or new growths on your skin are critical in detecting skin cancer at its earliest stage. If you notice any suspicious skin changes or have a family history of skin cancer, it’s essential to see a dermatologist as soon as possible.
Certain risk factors can increase your chances of developing skin cancer, such as prolonged sun exposure, tanning bed use, fair skin, a family history of skin cancer, and immune-suppressing drugs. If you’re concerned about your skin cancer risk, please speak with a dermatologist to learn more about prevention, early detection, and treatment options.
How to detect skin cancer?
Detecting skin cancer early is crucial for successful treatment. The best way to detect skin cancer is by regularly examining your skin for any changes or suspicious spots. You can do this by following the ABCDE rule, which stands for asymmetry, border irregularity, color variation, diameter larger than 6 millimeters, and evolving.
To perform a self-examination, use a well-lit room and a full-length mirror to examine your entire body, including your scalp, face, ears, neck, chest, abdomen, back, arms, legs, and the soles of your feet. Don’t forget to check hard-to-see areas like your back, buttocks, and the back of your legs by using a hand-held mirror or asking a family member or friend for help.
If you notice any suspicious spots or changes on your skin, such as a mole or lesion that has changed in size, shape, or color, or if you experience itching, bleeding, or oozing from a spot, make an appointment with a board-certified dermatologist immediately. They can perform a skin biopsy to determine if the spot is cancerous, and if so, recommend the best course of treatment.
Remember, prevention is key. Protect your skin from the sun by wearing protective clothing, using a broad-spectrum sunscreen with an SPF of 30 or higher, seeking shade, and avoiding tanning beds. Regular skin examinations and sun protection can help reduce your risk of developing skin cancer.
How common is skin cancer?
Skin cancer is the most common type of cancer in the United States. According to the American Academy of Dermatology, about 1 in 5 Americans will develop skin cancer by the age of 70. The Cleveland Clinic reports that around 20% of Americans will develop skin cancer sometime in their life. Additionally, the Skin Cancer Foundation states that more than 2 people die of skin cancer in the U.S. every hour.
Having five or more sunburns in your life doubles your chance of developing melanoma. Therefore, it’s important to take measures to protect your skin from the sun, such as wearing protective clothing and using sunscreen with at least SPF 30.
If you’re concerned about the risk of skin cancer or have noticed any changes in your skin, It is recommended to consult with a board certified dermatologist for a full skin examination. Early detection and treatment are key to successfully managing skin cancer. D. Rokhsar is double board certified in dermatology and mohs micrographic dermatologic surgery. Dr. Rokhsar is an experienced skin cancer surgeon.
How to prevent skin cancer?
It is recommended to wear sunscreen as a crucial part of preventing skin cancer. You should wear a broad-spectrum (UVA/UVB) sunscreen with an SPF of at least 15 every day, and for extended outdoor activity, use a water-resistant, broad-spectrum (UVA/UVB) sunscreen with an SPF of 30 or higher. Apply 1 ounce (2 tablespoons) of sunscreen to your entire body 30 minutes before going outside.
In addition to sunscreen, you should also avoid direct sunlight as much as possible during peak sun hours, generally from 10 a.m. to 3 p.m. Seek shade during this part of the day, and wear protective clothing like wide-brimmed hats and long-sleeved shirts. Protection from UV rays is important all year, not just during the summer months.
Aside from protection, incorporating certain vitamins and antioxidants into your diet can also help prevent skin cancer. Vitamins C, E and A, zinc, selenium, beta carotene (carotenoids), omega-3 fatty acids, lycopene, and polyphenols are among the antioxidants many dermatologists recommend including in your diet.
Lastly, it’s important to perform regular self-examinations of your skin and visit a dermatologist for a professional skin examination at least once a year. Early detection of skin cancer gives you the greatest chance for successful treatment. If you have a history of skin cancer or other risk factors, you may need to be seen more frequently.
How is skin cancer treated?
Skin cancer treatment options vary based on the type of skin cancer, its stage, size, and location, as well as its features. The most common skin cancers are basal cell carcinoma, squamous cell carcinoma, and melanoma.
For basal cell and squamous cell carcinoma, surgical removal or electrodesiccation and cautery of the cancer is often all that is needed. Mohs surgery is considered the most precise and accurate way to treat skin cancer with the highest cure rates and least scarring. Dr. Rokhsar is a double board certified Mohs surgeon who specializes in surgical treatment of skin cancer through Mohs surgery. Photodynamic therapy, biological therapy, and radiation therapy are also effective options for treating skin cancer that has spread to other parts of the body. Additionally, drug therapies like chemotherapy and targeted therapy drugs are recommended for some patients.
Melanoma skin cancer is more aggressive than basal cell and squamous cell carcinoma, and its treatment options are also more extensive. Based on the stage of the cancer and other factors, your treatment options might include surgery through wide surgical excision, immunotherapy, targeted therapy drugs, chemotherapy, and radiation therapy.
What is Mohs reconstruction surgery?
Mohs reconstruction surgery is a procedure that is performed after Mohs surgery to remove skin cancer. Mohs surgery is a highly effective technique for treating many types of skin cancer, including basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs). During Mohs surgery, thin layers of skin are removed and examined under a microscope until all the cancer cells are removed.
After Mohs surgery, there may be a wound that requires reconstruction. Mohs reconstruction surgery is the process of repairing the wound to restore the appearance of the skin. This procedure is often performed by a dermatologic surgeon who has specialized training in Mohs reconstruction. Dr. Cameron Rokhsar is a board certified Mohs surgeon with many years of experience in reconstruction of skin cancer defects.
The reconstruction process may involve a variety of techniques, depending on the size and location of the wound. The surgeon may use skin grafts, flaps, or sutures to close the wound and restore the appearance of the skin. The goal is to achieve a natural-looking result that blends seamlessly with the surrounding skin.
The healing process after Mohs reconstruction surgery can vary depending on the extent of the procedure. In general, patients can expect some swelling, bruising, and discomfort in the area for several days after the procedure. It is important to follow the surgeon’s instructions for post-operative care to ensure proper healing.
If you have been diagnosed with skin cancer and are considering Mohs surgery, it is important to discuss the reconstruction process with your surgeon. They can provide you with more information about the procedure and help you understand what to expect during the healing process. It is also important to choose a surgeon with extensive experience in Mohs reconstruction surgery to ensure the best possible outcome.
Who performs Mohs surgery?
Mohs surgery is a specialized procedure used to treat skin cancer. It is performed by dermatologists who have received specialized training in Mohs surgery and fulfill three roles: as the surgeon who removes the cancerous tissue, as the pathologist who analyzes the lab specimens, and as the surgeon who closes or reconstructs the wound.
Most Mohs surgeons are dermatologists who have completed extensive training in Mohs surgery. When looking for a doctor to perform Mohs surgery, it is important to find a board-certified dermatologist who is also board certified in Mohs micrographic surgery and who performs Mohs surgery on a regular basis. The more experience a doctor has performing Mohs surgery, the better prepared he or she is to anticipate and prevent complications. Dr. Rokhsar has 20 years of experience in Mohs surgery and reconstruction and is board certified in dermatologic micrographic surgery.
Mohs surgery requires the doctor to cut away the diseased tissue a bit at a time, so it is a time-consuming process that can take several hours. During the surgery, an anesthetic will be injected into the area where the tumor is located, numbing it completely and making the surgery painless. Most patients remain awake and alert during the procedure, and it can safely be performed in a medical office or surgical suite.
How long does Mohs surgery take?
The duration of Mohs surgery varies from patient to patient. The procedure can take anywhere from three to five hours, with some cases taking longer. Each stage of the surgery can last between 30 to 90 minutes, and if necessary, multiple stages may be required to remove all cancerous tissue. The healing process following Mohs surgery can take up to 18 months, with scars continuing to heal during that time. Dr. Rokhsar can always resurface scars with lasers to further improve the appearance of scars following Mohs surgery.
While infections are rare, they can occur following Mohs surgery. Symptoms such as increased redness, tenderness, swelling, and drainage may indicate an infection, and patients should contact their doctor immediately if they notice any of these symptoms. Stitches are typically removed within 7 to 14 days of the procedure, although the timing may vary depending on the location of the incision. It is recommended that patients refrain from strenuous activities in the first 1-2 weeks following the procedure to avoid post-operative wound reopening, which may lead to bleeding, infection, and significant scarring.
If you are considering Mohs surgery, it is important to discuss the procedure and potential risks with a board-certified dermatologist or Mohs surgeon. Each patient’s situation is unique, and a thorough evaluation is necessary to determine the best treatment plan for your specific needs.
How much does Mohs surgery cost?
The cost of Mohs surgery varies depending on various factors, including the experience of the doctor, the location of the practice, the complexity of the case, and whether you have insurance coverage.
It’s also important to consider that other skin cancer treatment methods might require additional surgeries and pathology readings to treat the cancer if it’s not completely removed, and all of these require separate fees. That’s why Mohs surgery is often the preferred method for treating skin cancer, as it has the highest cure rate of any skin cancer treatment option.
If you’re considering Mohs surgery, Dr. Rokhsar recommends consulting with a double board-certified dermatologist and dermatologic surgeon who specializes in this procedure. They can give you an accurate estimate of the cost based on your individual case and insurance coverage.
How to bandage a nose after Mohs surgery?
Firstly, after Mohs surgery, you should leave the bandages on for at least 24 hours, depending on the specific instructions from your surgeon. You should also follow up by cleansing the wound with soap and water and covering it with ointment and a dressing outside.
In some cases It is recommended for the bulky dressing to be left on for 24 hours. After that, you can clean the wound with hydrogen peroxide and use Q-tips dipped in the solution to gently remove any scabs or old blood. Once the wound is cleaned and dry, you can apply a layer of Vaseline petroleum jelly or Aquaphor to it and then cover it with a new bandage.
If the surgical site is on your face, you should sleep with your head elevated on two pillows or in a recliner and avoid sleeping on the affected side. Every case is unique, and your surgeon may provide you with specific instructions for how to bandage your nose after Mohs surgery based on your individual situation. Therefore, it’s important to follow their instructions closely to ensure proper healing and minimize the risk of complications.
How long does Mohs surgery take to heal?
The length of time it takes to heal after Mohs surgery can vary depending on the size and location of the wound. Typically, stitches are removed within 7 to 14 days after the procedure, but it may take up to 12 weeks for the treatment area to completely heal.
During the first few days after surgery, it is common to experience some bruising, swelling, and discomfort. However, these symptoms should gradually subside as your body begins to heal. It is important to follow your surgeon’s post-operative instructions carefully to ensure proper healing and minimize the risk of complications.
After Mohs surgery, it is also important to be patient as your scar continues to heal over the next 12 to 18 months. While the scar may initially appear red and swollen, it should gradually fade over time. If you are unhappy with your scar, talk to your surgeon about your options for scar revision and laser resurfacing with the CO2 or Fraxel lasers.
If you have been advised in the past to take antibiotics before a surgical procedure, such as dental work, please adhere to the prescription instructions before your Mohs surgery appointment.
What Is The Mohs Surgery Healing Process Like?
An indefinite follow-up period of observation is necessary after the wound has healed. You will be asked to return in six weeks, six months, and one year following the procedure. Studies have also shown that once you develop skin cancer, there is a strong possibility of developing other skin cancers in the future. Should you notice any suspicious areas, it is best to check with your physician for a complete evaluation. You will be reminded to return to your dermatologist on a frequent basis for continued evaluation of your skin.
New York Office Locations
Upper East Side Manhattan Office
121 East 60th Street, Suite 8AB New York, NY 10022
(212) 285-1110
Long Island Office
901 Stewart Ave, Suite 240, Garden City, NY 11530
(516) 512-7616



 Dr. Rokhsar was chosen by
Dr. Rokhsar was chosen by 






